Improving Outcomes Can Decrease Healthcare Cost
How many days a week and times a day do you read or hear something related to healthcare cost and spending? Almost every healthcare feed I receive includes a section on this topic. The work of the Hospital Engagement Networks with the Partnership for Patients is partly about reducing healthcare cost and primarily about improving care and outcomes of care.
The outcome goals are to reduce hospital acquired conditions by 40% and readmissions by 20%, but the bottom line is always part of the focus as well. When hospital stays are not prolonged due to hospital acquired conditions and patients are provided appropriate care transitions thereby preventing an additional hospitalization within 30 days the health and wellbeing of the patient is improved and no additional cost is incurred to the insured, insurer, family, etc.
The North Texas region has been working on reducing readmissions for many years and that is shown by the lower readmission rates within this area as compared to the national rate. Readmissions are tracked for patients admitted with Heart Attack (Acute Myocardial Infarction or AMI), Congestive Heart Failure (CHF) and Pneumonia as these are identified by CMS as the most likely to readmit within 30 days.
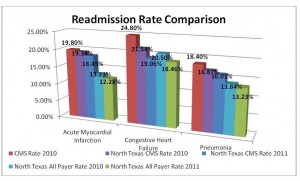
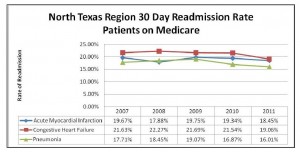
The most recent aggregate data from CMS for readmissions is from 2010. This chart shows that patients’ on Medicare (CMS) have higher incidence of 30-day readmissions than when all patients are included. Younger patients, even with these hospitalizations, are less likely to be readmitted within 30 days. The North Texas region has a lower rate of readmission for all three diagnoses in 2010 as compared to the national rate. The North Texas readmissions are improved further from 2010 to 2011!
AHRQ provides mean charges for hospitalizations based on diagnosis related group through the Healthcare Cost and Utilization Project (HCUP).

http://hcupnet.ahrq.gov/
Based on the mean charges for each diagnosis the approximate savings produced by our North Texas hospitals through their reduction in readmissions from 2010 to 2011 is $9 million.
When outcomes are improved through providing better care, improving care transitions and involving patients and families in their care, dollars are saved and that is a positive outcome as well.
